An angiogram is a special form of x-ray that permits the diagnosis of blockages (occlusions) or narrowing (stenosis) in the arteries of the body. During the test, a tube (catheter) is inserted into an artery at the groin. A special radio-opaque dye (contrast medium) is injected down the tube and x-ray pictures are taken as the solution passes along the blood vessels. Sometimes, when your kidneys are not functioning too well, your doctor might use CO2 (Carbon Dioxide gas) as a contrast medium for the procedure as this gas is removed thru the lungs and does not affect the kidneys. The whole procedure usually lasts approximately one hour. The arteries take blood from the heart to supply oxygen to muscles and organs and the angiogram will tell your doctor if the supply of blood is abnormal. The procedure is performed by a specialist vascular surgeon.
You will normally be admitted to the ward for a few hours/one day beforehand to check out your general health and to prepare you for the angiogram. On the day of the test you may eat and drink as normally till the nurse advises you to stop or oral foods/liquids. . If you take regular medications you should take your usual morning doses. If you have diabetes and inject insulin you should have your normal food and insulin dose, unless instructed not to. On arrival, you will be seen briefly by the doctor, the test will be explained to you and you will be asked to sign a consent form. This is to ensure you understand the test and its implications. Please tell the doctor if you have had any allergies or bad reactions to drugs or other tests. It would also be helpful to mention to the doctor if you have asthma, hay fever, diabetes, or any heart or kidney problems. Kidney problems can be particularly important. This is because the dye used to outline the arteries can damage the kidneys if special precautions are not taken. If you have any worries or queries at this stage don't be afraid to ask. The staff will want you to be as relaxed as possible for the test and will not mind answering your queries. You will be asked to put on a hospital gown. The test will take place in the Cath Lab department of the hospital; a nurse will escort you and stay with you during the test. A small drip will be placed into a vein in the arm or hand during the procedure. This may be used to give intravenous fluids. It may be necessary to trim some of the hair from the groin area before the test to help skin cleaning.
Your vascular surgeon will inject a local anesthetic into the skin at the groin "freezing" the area. After this injection the procedure should be fairly painless. The long fine tube (catheter) is then inserted into the artery at the groin (common femoral artery), and using x-rays to help, your vascular surgeon manipulates the catheter into the correct position. You will not feel the catheter being moved around your body.
X-ray pictures are taken whilst the dye is injected down the catheter into the blood vessels. To be able to take pictures along a length of arteries, your vascular surgeon will move the bed so that different portions of the arteries can be examined. Sometimes angiograms are also performed by placing a catheter in the arteries of the arm (brachial or axillary angiogram). Some injections may cause hot flushing for a few seconds, and an occasional feeling of wanting to pass urine. When the test is completed the catheter is removed and pressure will be applied to the groin for approximately ten minutes to minimize any bruising. Sometimes small devices can be deployed into the puncture site to seal the hole more quickly.
You will be taken back to the ward to rest for a few hours. It is important that you lie quietly so that the groin does not bleed again. The nursing staff will check the groin, and foot pulses at regular intervals. If no pulses are present the color and temperature of the foot is important. Providing all is well, you will be allowed home, but you need someone with transport to take you home, or to accompany you in a taxi. Some patients do require overnight stay. It is important that you rest completely until the next day to ensure that the puncture site in the groin heals up. If after you get home you notice any swelling or bleeding at the puncture site, you should press on this and call your GP's surgery for advice.
The vascular surgeon will look at the x-ray pictures and discuss their findings. They will decide the best form of treatment for you. Usually, the choice will be between an angioplasty, a bypass,or only treating with medicines .The patient can decide whether to proceed with treatment or not. For most patients these days, angioplasty will be performed at the same time as angiography and so there will be no need to return for a further procedure.
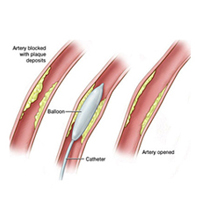
An angioplasty is a procedure where a balloon is passed into your artery on the end of a tube (catheter) and is inflated (blown up) to treat a narrowed or blocked artery. The angioplasty technique means that surgery may be avoided in many cases. As far as the patient is concerned, angioplasty is very similar to an angiogram except that a slightly bigger catheter is used and therefore the risks of bleeding are slightly greater. For this reason, in most cases, you will be asked to stay overnight. You will usually be asked to start taking aspirin before you are admitted as this makes the blood less sticky. If you have a stomach ulcer or are allergic to aspirin, please tell your doctor.
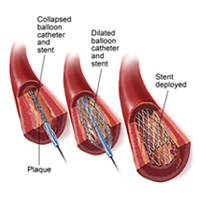
Angioplasty takes a little longer than simple angiography and you may feel the doctor changing, and pushing, catheters in and out of your groin artery. Although this is occasionally a little uncomfortable, it is not usually too painful. Once in position the artery will be stretched by inflating the balloon. This is a special balloon that will only inflate to a fixed diameter which will vary depending on the size of the artery being treated. The reason for this is that the fixed diameter prevents over inflation of the balloon and reduces the risk of rupturing the artery. If there appears to be a good angiographic result no further procedures may be necessary. Sometimes, if the appearance of the treated artery is not ideal the situation can be improved or salvaged by inserting a special device called a stent to keep the artery open. This is just a small metal tube that expands in your artery to keep the area open and allow more blood to flow through.
Recently, vascular surgeons have started using drug coated balloons and stents for certain situations. The drug release from these device into the blood vessel wall has been shown to improve success rates for angioplasties.
Unless there is a contraindication most patients should be taking aspirin. In some cases Heparin injections (anticoagulation) will be given for 24 hours to prevent the blood clotting at the site of the angioplasty. Rarely may you require Warfarin or similiar tablets to thin the blood for a few months. You will normally be allowed home the following day. If you are given heparin or Warfarin this may delay your departure by a few days. There is a growing trend to use clopidogrel to improve angioplasty success in leg arteries as it does seem to be important in patients undergoing coronary angioplasty in the heart. It is important to check whether you are allowed to drive after angioplasty.
You will be seen again in the clinic by your surgeon to assess the success of the angioplasty and to decide upon any further treatments.
Unfortunately, in about 10% of cases, angioplasty is not successful and other treatments will need to be considered. In addition, even where successful angioplasty has been performed, there is a risk that the area in the artery will narrow down again.
After one year, about 20-40% of arteries will have re-narrowed. In some cases, it may be possible to repeat the angioplasty at that time although in others this may not be possible. Very rarely, if angioplasty does not work, the circulation may actually worsen. If this is a particular risk in your case, your surgeon will discuss the risks with you.
One must remember however that a leg artery angioplasty is very often meant to heal a wound in the leg, and once that is achieved, the artery closing down again might not cause that many symptoms as when the wound was present.
You cannot do anything to relieve the actual narrowing in your arteries. However, you can improve your general health by taking regular exercise, stopping smoking, keeping your blood sugar under check and reducing the fat in your diet. Your blood pressure should also be measured and kept under control. These actions will help slow down the hardening of the arteries which caused the problem in the first place, and may avoid the need for further treatment in the future.
The effectiveness of angioplasty depends on exactly which type of angioplasty is performed. In general if the artery is only narrowed, and has not totally blocked, then angioplasty is more likely to be successful and any improvement is likely to last longer. If the length of artery to be treated is short (less than 5cms), then angioplasty is likely to be more successful than if a much longer length of artery is diseased and requires treatment. Angioplasty is more likely to be successful in a large artery (iliac arteries in pelvis) versus a small artery (tibial arteries in calf). Other factors that may be important are the amount of plaque and degree of calcification present. Apart from technical issues related to the angioplasty, factors such as diabetes and thrombophilia are important in ongoing benefits from angioplasty. If you continue to smoke it is more likely that and angioplasty will not be successful. Overall angioplasty is technically successful in 90-100% of patients, though long term success rates vary from person to person depending on various factors such as after care, compliance with medications and lifestyle changes and the inherent nature of arterial disease to progress in time.